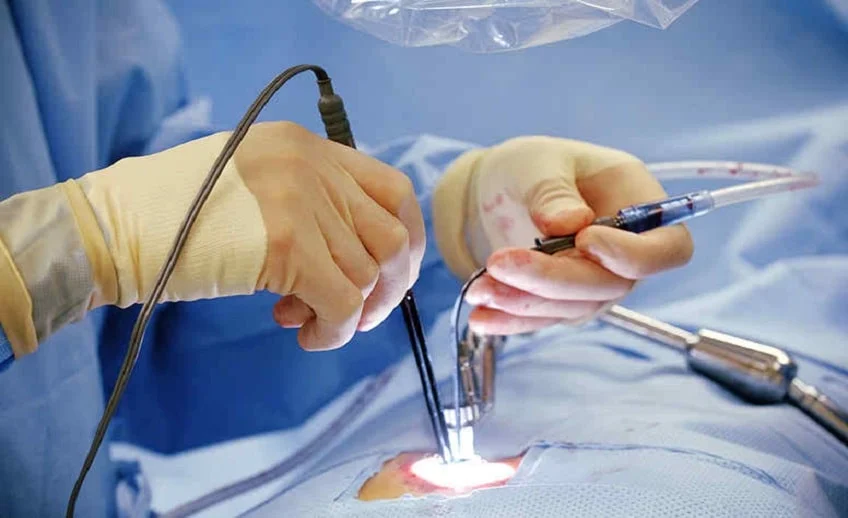
Endoscopic Spine Surgery is an advanced minimally invasive spine procedure designed to treat a wide range of spinal disorders with minimal disruption to surrounding tissues. Unlike traditional open spine surgery, this technique uses a thin endoscope equipped with a high-definition camera and specialized instruments inserted through a very small incision. The magnified visualization allows precise treatment of the affected spinal structures while preserving muscles, ligaments, and healthy bone. This approach significantly reduces postoperative pain, shortens hospital stay, and promotes faster recovery. Under the expertise of Dr. Raghu Samala, patients receive personalized, evidence-based care using the latest advancements in minimally invasive spine surgery to restore mobility and improve quality of life.
Endoscopic spine surgery is recommended when spinal conditions cause persistent symptoms that do not improve with conservative treatment. Common underlying causes include herniated (slipped) discs, spinal stenosis, degenerative disc disease, nerve root compression, and certain cases of spinal instability. Age-related wear and tear, prolonged poor posture, heavy physical work, trauma, or repetitive strain may contribute to these conditions. When inflammation or structural changes in the spine compress nearby nerves, surgical intervention may be necessary to relieve pressure and restore function.
Patients who may benefit from endoscopic spine surgery often experience chronic back pain or neck painthat radiates into the arms or legs. Symptoms can include numbness, tingling, muscle weakness, or difficulty walking due to nerve compression. Sciatica, characterized by sharp shooting pain down the leg, is a common presentation in lumbar disc problems. In some cases, patients report worsening pain with prolonged sitting, standing, or movement. When these symptoms persist despite medications, physiotherapy, and lifestyle modifications, surgical evaluation becomes important.
A comprehensive diagnosis begins with a detailed medical history and neurological examination. Imaging studies such as MRI scans are essential to identify disc herniation, spinal stenosis, or other structural abnormalities causing nerve compression. CT scans or X-rays may also be used to assess bone alignment and spinal stability. Accurate imaging allows precise localization of the problem, ensuring that endoscopic spine surgery is appropriately planned and targeted to the affected area.
Endoscopic spine surgery focuses on relieving nerve compression and correcting structural abnormalities through a minimally invasive approach. During the procedure, a small incision—often less than one centimeter—is made, and the endoscope provides real-time visualization of the spine. The surgeon carefully removes herniated disc fragments, trims excess bone, or addresses other sources of compression while preserving normal anatomy as much as possible.
This technique is particularly effective for lumbar and cervical disc herniations and selected cases of spinal stenosis. In suitable candidates, it offers comparable results to open surgery with less tissue trauma. Dr. Raghu Samala carefully evaluates each patient to determine whether endoscopic spine surgery is the most appropriate and safest option based on the severity and location of the condition.
Recovery after endoscopic spine surgery is typically faster compared to conventional procedures. Many patients are able to walk within hours of surgery and return home the same day or after a short hospital stay. Postoperative care includes gradual return to normal activities, pain management, and a structured physiotherapy program to strengthen spinal muscles and improve flexibility. Regular follow-up visits and imaging, when necessary, ensure proper healing and long-term success of the procedure.
Although endoscopic spine surgery is considered safe and minimally invasive, it carries potential risks similar to any surgical procedure. These may include infection, bleeding, nerve irritation, recurrence of disc herniation, or incomplete symptom relief. However, due to smaller incisions and limited tissue disruption, the overall risk profile is lower than traditional open surgery. Careful patient selection, meticulous surgical technique, and postoperative monitoring significantly reduce complications.
You should consult a spine specialist if you experience persistent back or neck pain lasting more than a few weeks, especially if accompanied by radiating pain, numbness, weakness, or difficulty walking. Sudden worsening of neurological symptoms or loss of bladder and bowel control requires immediate medical attention. Early evaluation allows timely intervention and prevents long-term nerve damage. Scheduling a consultation with Dr. Raghu Samala ensures expert assessment, accurate diagnosis, and access to advanced minimally invasive spine treatment options tailored to your needs.